Breaking Myths, Ending Stigma, and Acting Against Cervical Cancer
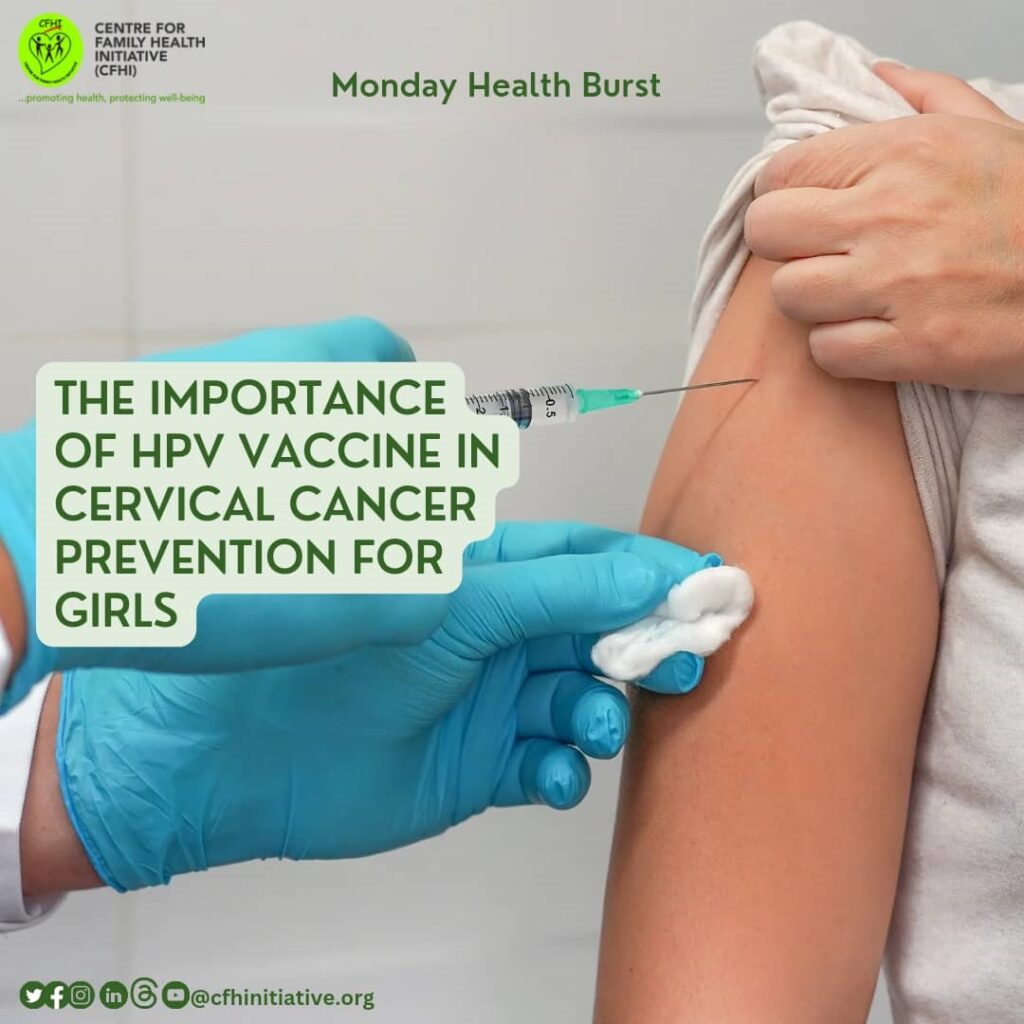
Cervical cancer is a major global health issue yet one of the most preventable forms of cancer. Almost all cervical cancer cases (about 99%) are linked to infection with high-risk human papillomaviruses (HPV), which are extremely common and transmitted through sexual contact. Persistent HPV infection can cause cervical cancer if left untreated, but early detection and prevention make this disease largely preventable. ¹
Despite this, myths and misinformation persist and contribute to stigma around cervical cancer screening and HPV. Studies show that many women feel shame, anxiety, and embarrassment when diagnosed with HPV or advised to get screened, often because HPV is incorrectly perceived as a sign of promiscuity or extreme risk. ² This stigma can deter women from seeking preventive care and early diagnosis, undermining efforts to reduce disease burden. ³
Globally, cervical cancer remains a leading cause of cancer deaths among women. In 2022, an estimated 660,000 new cases were diagnosed worldwide, with about 350,000 deaths many of which could be prevented through vaccination, regular screening, and early treatment. ¹ In Nigeria, cervical cancer is the second most common cancer among women and carries significant risk in the reproductive age group. ⁴
Despite proven benefits, uptake of cervical cancer screening and HPV vaccination remains low. Studies in Nigeria (2021–2023) show that fewer than 15% of adolescent girls have received the HPV vaccine and only about 10% of women have ever been screened, indicating slow progress compared to global targets.⁵ This low uptake is driven by limited awareness, misconceptions, stigma, and weak family or partner support, while reviews from 2022–2024 highlight persistent beliefs that screening is only for certain women or may cause harm, further discouraging participation.⁶
Myths about cervical cancer include beliefs that HPV always leads to cancer, that only women with symptoms should screen, or that screening itself causes harm. Evidence shows these are false HPV does not always cause cancer, early stages of disease often have no symptoms, and regular screening (Pap tests or HPV testing) is safe and effective in detecting abnormalities before they progress. ⁷
Stigma further compounds the problem. Surveys indicate that significant numbers of women experience emotional distress or feel ashamed after receiving abnormal screening results, which can delay follow-up care and discourage others from attending future screenings. ² Overcoming this stigma requires not just medical interventions but community education and open conversations about HPV and cervical health.
Acting against cervical cancer involves three key strategies: vaccination, screening, and treatment. The World Health Organization’s global strategy targets HPV vaccination of 90% of girls by age 15, screening 70% of eligible women twice in their lifetimes, and ensuring 90% of women with pre-cancer or invasive cancer receive appropriate care. ⁴ Countries such as Pakistan have demonstrated wide vaccination coverage, with campaigns reaching millions of girls despite resistance fueled by misinformation.
Breaking myths and ending stigma is essential to increase screening uptake and vaccine acceptance. Community education campaigns, trusted health messaging, and culturally sensitive outreach can help shift perceptions, build trust, and empower women to take preventive action. We urge communities, health workers, and families to actively support women in accessing screenings and vaccinations, speak openly about cervical health, and challenge harmful myths whenever they arise. When women understand the facts and feel supported rather than judged, lives can be saved, and the stigma that hinders progress can be dismantled.
References
- World Health Organization (WHO). Cervical cancer prevention, diagnosis, screening.
https://www.who.int/cancer/prevention/diagnosis-screening/cervical-cancer/en/ - Sheena Meredith. HPV stigma leads to shame for women with diagnosis. Medscape.
https://www.medscape.com/viewarticle/HPV-Stigma-Leads-Shame-Women-Diagnosis-2022a10004lc - BMC Public Health. Barriers to cervical cancer screening in Africa.
https://bmcpublichealth.biomedcentral.com/articles/10.1186/s12889-024-17842-1 - WHO Africa. Cervical cancer early detection saves lives (Nigeria context).
https://www.afro.who.int/countries/nigeria/news/cervical-cancer-early-detection-saves-lives - BMC Women’s Health. Cervical cancer screening and HPV vaccination knowledge in Nigeria.
https://bmcwomenshealth.biomedcentral.com/articles/10.1186/s12905-023-02345-9 - PubMed Central. Cervical cancer stigma—a silent barrier to elimination.
https://pmc.ncbi.nlm.nih.gov/articles/PMC11869935/ - Thomson Medical. 9 common myths about cervical cancer debunked.
https://www.thomsonmedical.com/blog/myths-about-cervical-cancer
Breaking Myths, Ending Stigma, and Acting Against Cervical Cancer Read More »