MONDAY HEALTH BURST
ENDOMETRIOSIS – CAUSES, SYMPTOMS, AND TREATMENT

Endometriosis, sometimes called “Endo,” is a common health problem in women. It gets its name from the word endometrium, the tissue that normally lines the uterus or womb. Endometriosis happens when tissue similar to the lining of the uterus (womb) grows outside of the uterus and on other areas in the body where it does not belong. It is especially common among women in 30s and 40s and may make it harder to get pregnant. Endometriosis is often found on the ovaries, fallopian tubes, tissues that hold the uterus in place or outer surface of the uterus.
The cause of Endometriosis is yet unknown, However, there are several theories associated with the causes of Endometriosis. The widely accepted theory is that the womb lining does not leave the body properly during a period and embeds itself on the organs of the pelvis. This is known as retrograde menstruation. Other factors include
- Genetic factors -Because endometriosis runs in families, it may be inherited in the genes.
- Immune system problems -A faulty immune system may fail to find and destroy endometrial tissue growing outside of the uterus. Immune system disorders and certain cancers are more common in women with endometriosis.
- Hormones -the hormone estrogen appears to promote endometriosis. Research is looking at whether endometriosis is a problem with the body’s hormone system.
- Surgery -during a surgery to the abdominal area, such as a Cesarean (C-section) or hysterectomy, endometrial tissue could be picked up and moved by mistake. For instance, endometrial tissue has been found in abdominal scars.
Endometriosis is a long-term (chronic) condition. Symptoms can vary significantly from person to person and some women have no symptoms at all. Yet, the most common symptoms include: painful periods or heavy periods which gets worse overtime; pain in the lower abdomen, pelvis or lower back, pain during and after sex, bleeding between periods, difficulty getting pregnant, painful bowel movements or pain when urinating during menstrual periods. Most women with endometriosis get pain in the area between their hips and the tops of their legs. Some women experience this pain all the time.
Other symptoms may include persistent exhaustion and tiredness, discomfort when defecating, bleeding from the back passage (rectum) or blood in feces, and coughing blood in rare cases when the endometriosis tissue is in the lung. How severe the symptoms are depends on where in the body the abnormal tissue is, rather than the amount of tissue present. A small amount could be more painful than a large amount. It is worthy of note that Endometriosis is rare in women who are in the menopause stage.
There is presently no cure for endometriosis. Endometriosis can be a difficult condition to deal with, both physically and emotionally but treatments are available for the symptoms and problems it causes. The symptoms of endometriosis can often be managed with painkillers and hormone medication, which help prevent the condition interfering with daily activities. Still, there is no known cure for endometriosis. For women who are not interested in getting pregnant, hormonal birth control is generally the first step in treatment. Patches of endometriosis tissue can sometimes be surgically removed to improve symptoms and fertility also. However, Surgery is usually chosen for severe symptoms, when hormones are not providing relief or if there are fertility problems.
Monday Health Burst is an initiative of CFHI to address issues of basic health concerns. Join us every Monday for more interesting episodes
MONDAY HEALTH BURST Read More »

 Child marriage is a widespread violation of human rights. It is an impediment to social and economic development, and it is rooted in gender inequality. The low value placed on girls and women brings about the act and acceptability of child marriage in societies where the practice is common. According to UNICEF, Child marriage refers to any formal marriage or informal union between a child under the age of 18 and an adult or another child. Child marriage is principally practiced in the rural and poor communities where young girls are regarded as economic burden and quickly married off to assuage household expenses.
Child marriage is a widespread violation of human rights. It is an impediment to social and economic development, and it is rooted in gender inequality. The low value placed on girls and women brings about the act and acceptability of child marriage in societies where the practice is common. According to UNICEF, Child marriage refers to any formal marriage or informal union between a child under the age of 18 and an adult or another child. Child marriage is principally practiced in the rural and poor communities where young girls are regarded as economic burden and quickly married off to assuage household expenses.





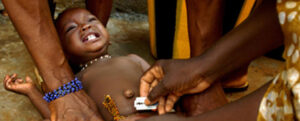 “Have you ever heard of Female genital mutilation? The doctor asked me. This was after my over 20 hours of labor, an ordeal which left me depressed for over a month. It took me a while before I responded because it was the least question I ever would imagine answering at such moment.
“Have you ever heard of Female genital mutilation? The doctor asked me. This was after my over 20 hours of labor, an ordeal which left me depressed for over a month. It took me a while before I responded because it was the least question I ever would imagine answering at such moment.

